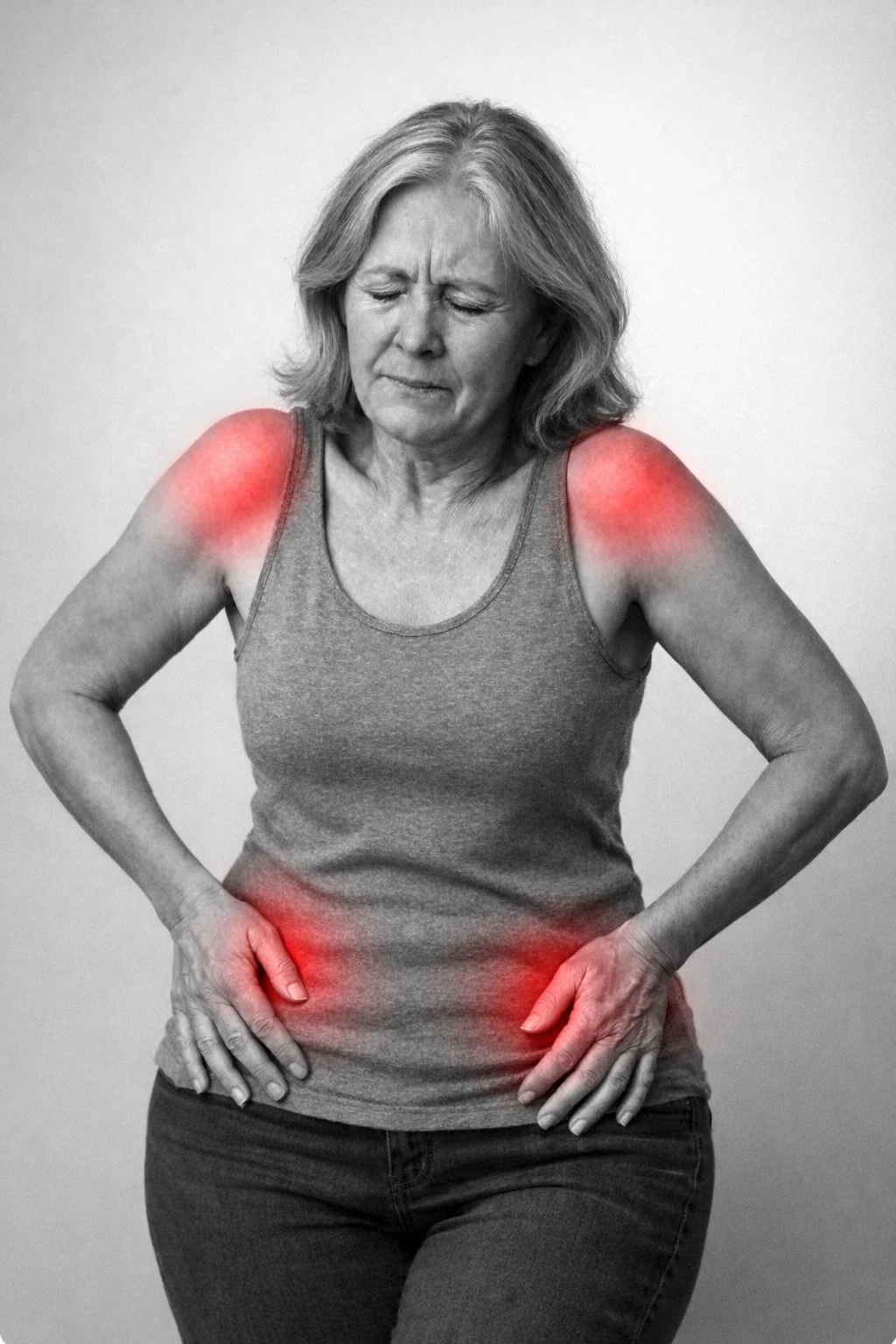
Polymyalgia Rheumatica (PMR) Explained: Symptoms, Diagnosis and Treatment
Polymyalgia rheumatica (PMR) is an inflammatory condition that causes pain, stiffness and marked functional difficulty, most commonly affecting people over the age of 50. Although it does not cause permanent joint damage, PMR can be profoundly disabling if not recognised and treated appropriately.
Many patients describe a sudden loss of independence — struggling to get out of bed, dress themselves, lift their arms, or stand from a seated position. When diagnosed promptly, however, PMR is a highly treatable condition.
What Is Polymyalgia Rheumatica?
PMR is a systemic inflammatory disorder that primarily affects the shoulder and hip girdles. The inflammation is not within the joints themselves, but in the surrounding soft tissues, leading to pain, stiffness and restricted movement.
It is closely related to giant cell arteritis (GCA), a more serious inflammatory condition affecting blood vessels, and the two can occur together.
(Related reading: Giant Cell Arteritis Explained)
Common Symptoms of PMR
Typical features include:
severe stiffness in the shoulders, upper arms, hips or thighs
difficulty raising the arms (e.g. combing hair, dressing)
stiffness that is worst in the morning and after rest
pain on movement rather than at rest alone
fatigue, fever or weight loss in some patients
Symptoms often develop over days to weeks and can be striking in their impact.
Diagnosis: Why Careful Assessment Matters
There is no single test that diagnoses PMR.
Diagnosis is based on:
a detailed clinical history
characteristic symptom patterns
examination findings
supportive blood tests showing inflammation
Blood markers such as ESR and CRP are often raised, but this is not diagnostic in isolation. Other causes of pain and stiffness — including inflammatory arthritis, infection or malignancy — must be considered and excluded where appropriate.
Clear explanation at this stage is crucial, as the diagnosis can feel unfamiliar and unsettling.
A Patient Experience
One patient described their experience of assessment and treatment for PMR as follows:
“I attended a consultation with Dr Singh to try to understand the reasons for the joint pains which I was suffering from. I found his knowledge and understanding of my symptoms and his ability to explain the reasons for my problem to be exemplary. He explained everything to me and without hesitation recommended a course of treatment which he felt would produce a long-term resolution of my problem. I have absolutely no hesitation in recommending him to anyone who wants to be treated by a doctor who has a first-class knowledge of his subject and who is capable of imparting this information in a format readily understandable to a non-medically trained patient. I can’t thank him enough for the relief which I am now enjoying.”
This reflects what many patients with PMR experience — significant symptoms, followed by meaningful improvement once the condition is recognised and managed appropriately.
Treatment of PMR
Steroids
Low to moderate doses of corticosteroids are the mainstay of treatment and usually lead to rapid improvement, often within days.
However, PMR is typically a longer-term condition, and treatment requires:
careful dose adjustment
gradual tapering
monitoring for relapse
attention to steroid side effects
(Related reading: Steroids in Rheumatology – Benefits, Risks and Sick Day Rules)
Methotrexate as a Steroid-Sparing Treatment in PMR
While corticosteroids remain the mainstay of treatment for polymyalgia rheumatica, methotrexate may be used in selected patients as a steroid-sparing agent. This is most commonly considered in individuals who experience repeated disease relapses, require prolonged steroid treatment, or develop significant steroid-related side effects.
Methotrexate is not required for most patients with PMR and is not used as first-line therapy. When introduced, it is used alongside steroids with the aim of improving disease control and supporting a more gradual and safer reduction in steroid dose over time. As with all disease-modifying treatments, its use requires appropriate monitoring and individualised decision-making.
(Related reading: DMARDs explained: methotrexate)
Monitoring and Long-Term Management
Although symptoms often respond quickly, PMR commonly requires treatment for 1–2 years, and sometimes longer.
Ongoing management focuses on:
balancing symptom control with steroid minimisation
monitoring inflammatory markers
watching for symptoms suggestive of GCA
protecting bone health
addressing steroid-related side effects
Relapses are common and do not mean treatment has failed — they are part of the natural course of the condition.
PMR and Giant Cell Arteritis
PMR and GCA are closely linked. A proportion of patients with PMR may develop GCA, which requires urgent assessment.
Symptoms that warrant immediate medical attention include:
new or severe headaches
scalp tenderness
jaw pain on chewing
visual disturbance
(Related reading: Giant Cell Arteritis Explained)
Please note, if you are concerned about GCA, please seek emergency medical review through your GP or A&E.
Why Specialist Input Is Helpful
PMR sits at the intersection of rheumatology and general internal medicine. Specialist assessment helps to:
confirm the diagnosis
exclude alternative causes
guide safe steroid use
manage relapses
minimise treatment complications
Clear explanation and continuity of care are particularly important in a condition that affects daily function and independence.
In Summary
PMR is a common inflammatory condition in older adults
It causes marked stiffness and loss of function
Diagnosis relies on careful clinical assessment
Steroids are effective but require thoughtful long-term management
Monitoring for GCA is essential
With appropriate care, most patients experience significant improvement
Trusted Patient Information Resources
Practical advice on managing symptoms, activity and long-term treatment.
https://www.arthritisuk.org/about-arthritis/conditions/polymyalgia-rheumatica/
PMR GCA UK
Polymyalgia and Giant Cell Arteritis UK are the only UK charity dedicated to patients with PMR/GCA
Please note, these posts are for general information only and do not constitute medical advice. Dr Singh would encourage you to speak to your healthcare professional to be assessed and managed for your specific symptoms.
If you are concerned that you or a relative has GCA, please seek emergency medical attention through A&E or your GP for assessment.